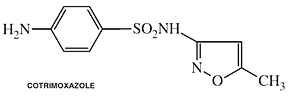

Cotrimoxazole
Please read the disclaimer concerning the intent
and limitations of the information provided here.
The information presented in Interactions is for
informational and educational purposes only. It is based on scientific
studies (human, animal, or in vitro), clinical experience, case
reports, and/or traditional usage with sources as cited in each
topic. The results reported may not necessarily occur in all
individuals and different individuals with the same medical conditions
with the same symptoms will often require differing treatments. For
many of the conditions discussed, treatment with conventional medical
therapies, including prescription drugs or over-the-counter
medications, is also available. Consult your physician, an
appropriately trained healthcare practitioner, and/or pharmacist for
any health concern or medical problem before using any herbal products
or nutritional supplements or before making any changes in prescribed
medications and/or before attempting to independently treat a medical
condition using supplements, herbs, remedies, or other forms of
self-care.
![]()
Do not rely solely on the information in this article.
References
Alappan, R, Perazella, MA, Buller, GK. Hyperkalemia in hospitalized patients treated with
trimethoprim-sulfamethoxazole. Ann Intern Med 1996;124:316-320.
Alappan R, et al. Trimethoprim-Sulfamethoxazole Therapy in Outpatients: Is Hyperkalemia a Significant Problem?
Am J Nephrol. 1999 May;19(3):389-394.
Bjornson BH, McIntyre AP, Harvey JM, Tauber AI. Studies of the effects of trimethoprim and sulfamethoxazole on human granulopoiesis.Am J Hematol
1986 Sep;23(1):1-7.
Abstract: Trimethoprim and sulfamethoxazole (Bactrim r) is a widely used antibiotic combination effective against a broad spectrum of microbial organisms. There are reports of neutropenia developing during even brief periods of oral therapy, particularly in individuals with either folate deficiency or increased folate requirements. We have investigated the effects of these drugs on circulating granulocyte precursors (CFU-C) from normal donors and the mechanism of inhibition on granulopoiesis using an in vitro CFU-C assay. In 12 healthy adults, the number of circulating granulocytes and granulocyte progenitors was not significantly altered by a 5-day course of therapy. However, in experiments that simulated the in vivo condition of folate deficiency (folate-free cultures were prepared with cells harvested from normal donors), trimethoprim (8 micrograms/ml) resulted in a 47% decrease in the total number of colonies; this inhibitory effect was prevented when 100 ng of folinic acid was also added to the culture. Sulfamethoxazole (40 micrograms/ml) had no discernible effect on granulopoiesis. The combination of 8 micrograms/ml of trimethoprim and 40 micrograms/ml of sulfamethoxazole resulted in a 52% decrease in the number of colonies generated and this inhibition was again prevented by folinic acid. Our results suggest that the neutropenia occasionally observed in patients treated with trimethoprim-sulfamethoxazole is due to the inhibitory effects on granulopoiesis by trimethoprim, namely its antifolate action, which is reversed by folinic acid. Based on these studies, in patients with either folate deficiency or increased folate requirements, trimethoprim-sulfamethoxazole should be used with caution.
Bugge JF. Severe hyperkalaemia induced by trimethoprim in combination with an angiotensin-converting enzyme inhibitor in a patient with transplanted lungs.
J Intern Med. 1996 Oct;240(4):249-251.
Bygbjerg IC, Lund JT, Hording M. Effect of folic and folinic acid on cytopenia occurring during co-trimoxazole treatment of Pneumocystis carinii pneumonia.
Scand J Infect Dis 1988;20(6):685-686.
Abstract: 12 AIDS/ARC patients with or suspected of Pneumocystis carinii pneumonia were treated with co-trimoxazole and received supplementary folic or folinic acid to avoid peripheral blood cytopenia. Most patients developed decreased numbers of neutrophils and hemoglobin while receiving co-trimoxazole. Supplementary folate/folinate could not abolish the drug-induced cytopenia. Routine prescription of folinic acid is not recommended. Folic acid is cheap and may be beneficial and should be prescribed.
Evers S, Di Padova K, Meyer M, Fountoulakis M, Keck W, Gray CP. Strategies towards a better understanding of antibiotic action: folate pathway inhibition in Haemophilus influenzae as an example.Electrophoresis 1998 Aug;19(11):1980-1988.
Abstract: Two-dimensional electrophoresis was applied to the global analysis of the cellular response of Haemophilus influenzae to sulfamethoxazole and trimethoprim, both inhibitors of tetrahydrofolate synthesis. Deregulation of the synthesis rate of 118 proteins, involved in different metabolic pathways, was observed. The regulation of the genes involved in the metabolism of the amino acids methionine, threonine, serine, glycine, and aspartate was investigated in detail by analysis of protein synthesis and Northern hybridization. The results suggested that the synthesis of methionine biosynthetic enzymes in H. influenzae is regulated in a similar fashion as in Escherichia coli. A good correlation between the results obtained by Northern hybridization and quantification of protein synthesis was observed. In contrast to trimethoprim, sulfamethoxazole triggered the increased synthesis of the heat shock proteins DnaK, GroEL, and GroES.
Kahn, SB, Fein, SA, Brodsky, I. Effects of trimethoprim on folate metabolism in man.
Clin Pharmacol Ther 1968;9:550-560.
Marinella MA. Trimethoprim-Induced Hyperkalemia: An Analysis of Reported Cases.
Gerontology. 1999 Jul;45(4):209-212.
Abstract: Background: Trimethoprim has been recently implicated in the development of hyperkalemia when administered at standard doses to immunocompetent patients. However, many clinicians are unaware of this potentially dangerous adverse effect. Objective: To review reported cases of trimethoprim-induced hyperkalemia in immunocompetent patients and identify predisposing factors, treatment, and outcome. Methods: A MEDLINE literature search was performed using the key words 'trimethoprim' and 'hyperkalemia'. All English-language case reports and bibliographies of immunocompetent patients with trimethoprim-induced hyperkalemia were reviewed. Results: Nine cases were identified. The mean patient age was 77.6 years, and the mean duration of therapy was 10.2 days. Seven patients received standard oral dosages of trimethoprim-sulfamethoxazole for common infections, and 2 patients were concurrently receiving angiotensin-converting enzyme inhibitors. The mean pretreatment levels of creatinine and potassium were 1.01 mg/dl and 4.55 mmol/l, respectively. The mean peak serum potassium level was 7.0 mmol/l. No deaths attributable to hyperkalemia occurred. Conclusions: Hyperkalemia due to trimethoprim typically affects elderly patients administered standard oral dosages, even in the presence of a normal serum creatinine level. Concurrent angiotensin-converting enzyme inhibitor therapy may increase the risk of hyperkalemia. The prognosis is favorable with standard therapy for hyperkalemia and withdrawal of trimethoprim.
Perazella MA. Hyperkalemia and trimethoprim-sulfamethoxazole: a new problem emerges 25 years later.
Conn Med. 1997 Aug;61(8):451-458. (Review)
Abstract: Trimethoprim-sulfamethoxazole is a frequently prescribed antibiotic with a wide spectrum of antimicrobial activity. A previously unreported and potentially lethal adverse reaction associated with "high dose" trimethoprim-sulfamethoxazole therapy, hyperkalemia, was described. Subsequent to the descriptions of hyperkalemia with "high dose" trimethoprim-sulfamethoxazole, a handful of cases noted the development of hyperkalemia with "standard dose" trimethoprim-sulfamethoxazole in elderly patients without evidence of an obvious defect in potassium homeostasis. A surveillance study of patients treated with "standard dose" trimethoprim-sulfamethoxazole as compared to similar controls treated with other antibiotics confirmed the rise in potassium associated with trimethoprim-sulfamethoxazole therapy. Recognition of this potassium disorder led to investigation and description of the mechanism by which trimethoprim-sulfamethoxazole-induced hyperkalemia. Trimethoprim was found to act like the potassium-sparing diuretic amiloride and reduce renal potassium excretion. Hence, trimethoprim-sulfamethoxazole therapy was found to be associated with a new adverse reaction, hyperkalemia, nearly 25 years after its introduction into clinical practice as an antimicrobial agent.
Perazella MA, et al. Trimethoprim-sulfamethoxazole: hyperkalemia is an important complication regardless of dose.
Clin Nephrol. 1996 Sep;46(3):187-192. (Review)
Perlmutter EP, Sweeney D, Herskovits G, Kleiner M. Case report: severe hyperkalemia in a geriatric patient receiving standard doses of trimethoprim-sulfamethoxazole.
Am J Med Sci. 1996 Feb;311(2):84-85.
Reiser IW, Chou SY, Brown MI, Porush JG. Reversal of trimethoprim-induced antikaliuresis.
Kidney Int. 1996 Dec;50(6):2063-2069.
Abstract: High-dose trimethoprim-sulfamethoxazole (TMP-SMX) causes hyperkalemia, thought to result from TMP-induced blockade of amiloride-sensitive Na(+)-channels in the distal nephron. The present study was performed in anesthetized dogs to determine if increasing distal sodium delivery affects this antikaliuretic effect. In Group 1, intrarenal infusion of vehicle did not alter renal function. In Group 2, i.v. infusion of amiloride led to diuresis, natriuresis and antikaliuresis associated with a reduction of the transtubular potassium gradient (TTKG) in both kidneys. Intrarenal infusion of TMP (0.2 mg/kg/min) into the left kidney did not further alter these parameters. In groups 3 and 4, intrarenal infusion of TMP caused an ipsilateral diuresis, natriuresis, antikaliuresis and a reduction in (TTKG) without affecting the contralateral kidney. The TMP infusion was followed by furosemide (20 mg i.v.) in group 3 and acute saline loading in group 4. Despite continuous TMP infusion, both furosemide and saline loading reversed the antikaliuretic effect of TMP in the ipsilateral kidney and was associated with a similar kaliuresis, diuresis, natriuresis and decrease in urine osmolality in both kidneys. The TTKG following furosemide or saline loading increased in the ipsilateral kidney and decreased in the contralateral kidney. In all groups the systemic and renal hemodynamics remained unchanged. These results suggest that acute administration of TMP inhibits the amiloride-sensitive Na(+)-channel and K+ secretion in the distal nephron. Maneuvers that increase distal Na+ delivery can abrogate TMP's antikaliuretic effect due, in part, to an increase of the low TTKG observed with TMP.
Witt JM, Koo JM, Danielson BD. Effect of standard-dose trimethoprim/sulfamethoxazole on the serum potassium concentration in elderly men.
Ann Pharmacother. 1996 Apr;30(4):347-350.
Abstract: OBJECTIVE: To determine the effect of standard-dose trimethoprim/sulfamethoxazole (TMP/SMX) (TMP 160 mg and SMX 800 mg q12h) on the serum potassium concentration. DESIGN: Retrospective and concurrent study. SETTING: A Veterans Affairs Medical Center. PATIENTS: Fifty-three men hospitalized at the Fargo Veterans Affairs Medical Center. Thirty-three patients who received standard-dose TMP/SMX for 3 or more days comprised the study group. Twenty patients who received oral cephradine or amoxicillin for 3 or more days comprised the control group. Patients who received potassium supplements, potassium-sparing diuretics, angiotensin-converting enzyme inhibitors, nonsteroidal antiinflammatory drugs, beta-blockers, heparin, known nephrotoxic agents, patients with a serum creatinine concentration of more than 177 mumol/L, and patients with baseline hyperkalemia (serum potassium concentration > 5.1 mmol/L) were excluded. RESULTS: The serum potassium concentration in the study group was 4.22 +/- 0.40 mmol/L and increased by 0.31 +/- 0.38 mmol/L at the end of therapy (p < 0.001). Twenty-six patients in the study group (78.8%) had an increase in the serum potassium concentration during TMP/SMX therapy. Fourteen of these patients had follow-up serum potassium concentrations obtained after completion of therapy. The serum potassium concentration returned to baseline in 10 of these patients. The serum creatinine concentration also increased during therapy. However, the correlation between the increase in the serum potassium concentration and the increase in the serum creatinine concentration was weak (Pearson r = 0.29). The serum potassium in the control group was 4.34 mmol/L and remained essentially unchanged during therapy. CONCLUSIONS: Therapy with standard-dose TMP/SMX is associated with a slight increase in the serum potassium concentration. Routine monitoring of the serum potassium concentration in patients who are treated with standard-dose TMP/SMX therapy is unnecessary. However, TMP/SMX should be considered as a possible cause of unexplained hyperkalemia in elderly patients receiving TMP/SMX therapy.