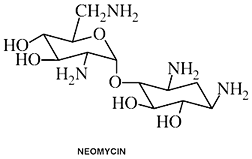

Neomycin
Brand Names: Minims, Neo-CortefPlease read the disclaimer concerning the intent
and limitations of the information provided here.
The information presented in Interactions is for
informational and educational purposes only. It is based on scientific
studies (human, animal, or in vitro), clinical experience, case
reports, and/or traditional usage with sources as cited in each
topic. The results reported may not necessarily occur in all
individuals and different individuals with the same medical conditions
with the same symptoms will often require differing treatments. For
many of the conditions discussed, treatment with conventional medical
therapies, including prescription drugs or over-the-counter
medications, is also available. Consult your physician, an
appropriately trained healthcare practitioner, and/or pharmacist for
any health concern or medical problem before using any herbal products
or nutritional supplements or before making any changes in prescribed
medications and/or before attempting to independently treat a medical
condition using supplements, herbs, remedies, or other forms of
self-care.
![]()
Do not rely solely on the information in this article.
References
Barrowman JA, Broomhall J, Cannon AM, Christmas S, D'Mello A, Herxheimer A, Pring DW, Robson TW, Woolf AD. Impairment of vitamin A absorption by neomycin.
Clin Sci. 1972 Apr;42(4):17P.
Cullen RW, Oace SM. Neomycin has no persistent sparing effect on vitamin B-12 status in pectin-fed rats. J Nutr.
1989 Oct;119(10):1399-1403.
Abstract: In the present study, rats were depleted of vitamin B-12 with fiber-free or 5% pectin diets, with or without neomycin. Through use of this intestinal antibiotic reported to "spare" vitamin B-12, we sought to determine if bacterial fermentation of pectin might explain our previous observations of negative effects of pectin on vitamin B-12 status. However, neomycin did not lessen interference by pectin with vitamin B-12 metabolism. Pectin increased urinary methylmalonate and decreased propionate oxidation to a greater extent in the presence than in the absence of neomycin. Also, regardless of the presence of neomycin, the biologic half-life of injected [57Co]vitamin B-12 was 58 d for rats fed the fiber-free diets and only 38 d for rats fed 5% pectin diets. Neomycin delayed early fecal excretion of 57Co but had no persistent effect. Thus, neomycin-sensitive bacteria do not mediate the negative effects of pectin on vitamin B-12 status. Pectin may interfere directly with vitamin B-12 absorption or may stimulate vitamin B-12 uptake or propionate production by microbial species that have adapted to neomycin.
Faloon WW, Paes IC, Woolfolk D, Nankin H, Wallace K, Haro EN. Effect of neomycin and kanamycin upon intestinal absorption.
Ann N Y Acad Sci. 1966 Jun 14;132(2):879-887.
Faloon WW. Metabolic effects of nonabsorbable antibacterial agents. Am J Clin Nutr. 1970 May;23(5):645-651.
Favaro RM, Silva HC, Vannucchi H. Bioavailability of vitamin A in the rat following ingestion of neomycin sulfate or aluminium hydroxide.
Int J Vitam Nutr Res. 1994;64(2):98-103.
Abstract: The objective of the present paper was to study the interaction of Neomycin and aluminium hydroxide with vitamin A in terms of the effect of these drugs on the bioavailability of vitamin A in the rat. Bioavailability was determined on the basis of the effects of the drugs on growth and on the plasma and hepatic levels of the vitamin. Vitamin A deficient animals were used in assay 1 and normal animals in assay 2. In each assay the animals were divided into 3 groups: one received Neomycin sulfate (0.1% in the diet), the second received aluminium hydroxide (0.05% in the diet) and the third (control) received no drug. Each of these three groups was subdivided into two groups receiving two different concentrations of vitamin A palmitate. The bioavailability of vitamin A was estimated by the parallel line method from the concentration of vitamin A in the diet and in the liver of the animals. No significant differences in growth or plasma retinol levels were observed between the groups of animals studied in assays 1 and 2. Total vitamin A concentration in the liver of the animals which received Neomycin was lower (p < 0.05) than that observed in the controls. Neomycin reduced the bioavailability of vitamin A by 13.9% (maximum, 18.1% and minimum, 9.6%) in assay 1 and by 13.5% (maximum, 17.7% and minimum, 9.3%) in assay 2. Aluminium hydroxide at the level tested did not affect the bioavailability of vitamin A.
Hardison WG, Rosenberg IH. The effect of neomycin on bile salt metabolism and fat digestion in man.
J Lab Clin Med. 1969 Oct;74(4):564-573.
Hill FW. An investigation of the effects of oral neomycin on intestinal absorption and serum cholesterol levels in the dog.
Br Vet J. 1973 Jul-Aug;129(4):337-44.
Holt GA. Food and Drug Interactions. Chicago: Precept Press, 1998, 183-184.
Kendall MJ, Chan K. Drug-induced malabsorption. Xenobiotica 1973 Nov;3(11):727-744. (Review)
Korolkiewicz Z, Pocwiardowska-Ciara E. Effect of ascorbic acid in the presence of neomycin on isolated rat stomach strips.
Acta Physiol Pol. 1986 Jul-Aug;37(4-5):177-182.
Abstract: The effects of vitamin C and acetylcholine on the smooth muscle of rat stomach were compared after neomycin-induced blockade of phosphatidylinositol metabolism. The cumulative curves of dose-dependent responses showed a non-competitive antagonism between vitamin C and neomycin. On the other hand, the antagonism between acetylcholine and neomycin was of a mixed, competitive-non-competitive type. The results of the experiments suggest the conclusion that a normal metabolism of phosphatidylinositol controlling calcium transport into the cells is necessary for the stimulating effect of vitamin C on the contractions of the smooth muscles in the digestive tract.
Lim KS, Huh CS, Baek YJ. Antimicrobial susceptibility of bifidobacteria. J Dairy Sci. 1993 Aug;76(8):2168-2174.
Abstract: The antimicrobial susceptibility of 37 strains of bifidobacteria to 18 antimicrobial agents was determined by a macrodilution broth method. Most of the strains used were isolated from commercial yogurts and starters. Tested organisms were usually sensitive to Gram-positive spectrum antibiotics (bacitracin, erythromycin, lincomycin, and vancomycin), and most of the organisms were inhibited by a concentration < 1.56 micrograms/ml. Erythromycin was the most active agent; all strains were inhibited by < .19 microgram/ml. beta-Lactam antibiotics (penicillin G, ampicillin, methicillin, and cephalothin), showing a wide range of minimum inhibitory concentration, were less effective than Gram-positive spectrum antibiotics. Most strains were somewhat resistant to cephalothin, exhibiting inhibition at concentrations of 6.25 to 25.0 micrograms/ml. Test organisms were most resistant to kanamycin, neomycin, paromomycin sulfate, nalidixic acid, and polymyxin B sulfate; inhibition occurred only at > or = 50 micrograms/ml, and strains were somewhat less resistant to gentamicin and streptomycin. Susceptibility to nitrofurantoin and tetracycline was variable; minimum inhibitory concentrations ranged from 1.56 to 50.0 and .39 to 50.0 micrograms/ml, respectively, but chloramphenicol had a narrow range from 1.56 to 6.25 micrograms/ml.
Linzenmeier G, Haralambie E, Dermoumi H. [Short-term oral chemoprophylaxis before intestine surgery. Quantitative determination of bacteria and fungi in stool specimens].
Zentralbl Bakteriol [Orig A] 1979 Apr;243(2-3):326-335. [Article in German]
Abstract: The methods of quantitative analysis of aerobe and anaerobe microbes and fungi stool specimens are described. The results of the studies in health people are compared to the results in patients undergoing surgical treatment of intestinal tract. A group of these patients received Neomycin and Bacitracin orally as short-time chemoprophylaxis to diminish possible woundinfection and/or sepsis. After oral medication germs as Bifidobacterium, Bacteroides and Clostridium (not Cl. perfringens) are reduced or lost, Veillonella, Eubacterium, Fusiformis, Peptostreptococcus and Lactobacillus were suppressed. Resistant strains of E. coli and Enterococci increased to high concentration/g faeces. After treatment the rate of gram-negative bacteria resistant to Neomycin increased. This might be of epidemiologically importance for the distribution of microbes resistant to Neomycin and other aminoglycosides as Klebsiella, Candida spec. and Torulopsis.
Matteuzzi D, Crociani F, Brigidi P. Antimicrobial susceptibility of Bifidobacterium.
Ann Microbiol (Paris). 1983 May-Jun;134A(3):339-349.
Abstract: The susceptibility pattern of 459 strains of bifidobacteria, representing 15 species, to 16 antimicrobial agents was determined by the broth dilution method. The majority of the strains derived from human faeces. Penicillin G, erythromycin, clindamycin, vancomycin and bacitracin were the most active compounds; they inhibited 90% of the strains at less than 1.6 micrograms/ml. All strains were susceptible to chloramphenicol (MIC90 = 2.0-5.8 micrograms/ml) and also to lincomycin (MIC50 = 0.64-1.5 micrograms/ml). Neomycin, streptomycin and tetracycline presented a great variability in their activity. Most strains were resistant to polymyxin B, nalidixic acid, kanamycin, gentamicin and metronidazole. The only variation in susceptibility which was observed among the different species concerned Bifidobacterium suis, which generally appeared to be more resistant than other species.
Mayer J. Iatrogenic malnutrition. Postgrad Med. 1971 Mar;49(3):247-249.
Olson JA. Recommended dietary intakes (RDI) of vitamin K in humans. Am J Clin Nutr. 1987 Apr;45(4):687-692.
Proskuriakova MG. [Effect of different food substances on the absorption of neomycin from the gastrointestinal tract in experimental animals].
Antibiotiki. 1970 Nov;15(11):1019-1021. [Article in Russian]
Race TF, Paes IC, Faloon WW. Intestinal malabsorption induced by oral colchicine. Comparison with neomycin and cathartic agents.
Am J Med Sci. 1970 Jan;259(1):32-41.
Ratnaike RN, Jones TE. Mechanisms of drug-induced diarrhoea in the elderly. Drugs Aging 1998 Sep;13(3):245-253.
Robinson C, Weigly E. Basic Nutrition and Diet Therapy. New York: MacMillan, 1984.
Roe DA. Diet and Drug Interactions. New York: Van Nostrand Reinhold, 1989.
Roe DA. Drug-induced Nutritional Deficiencies. 2nd ed. Westport, CT: Avi Publishing, 1985, 157-158.
Roe DA, Campbell T, eds. Drugs and Nutrients: The Interactive Effects. New York: Marcel Decker, 1984.
Salet J, Pean G, Hansel S, Baudon JJ. [Acute avitaminosis K in infants associated with diarrhea treated by antibiotics].
Arch Fr Pediatr. 1968 Oct;25(8):961. [Article in French]
Tuckerman M, Turco S. Human Nutrition. Philadelphia: Lea and Febiger, 1983, 215-222.